Cardiology Case #1
Primary Author: Dr Alastair Robertson; Co-Authors: Dr Hywel James and David Law
Background:
BAT call from ambulance: 65yo male, chest pain and STEMI criteria.
No reported significant PMHx, presented with persistent central chest pain for the last 20-24hrs.
Ambulance requesting to thrombolyse.
Initial ECG
-
Anterior STEMI with marked ST elevation V1-5 with associated Q waves suggesting established ischaemia. T-wave inversion in aVL. Concerning for large LAD occlusion.
QRS is broad around 120ms, with associated Left axis deviation/LAFB. If interpreted as LBBB this would still be positive for OMI by the Modified Sgarbossa criteria (STE >0.25x preceding S wave in V2-4).
Cardiac POCUS
Apical 4 chamber, Apical 2-chamber, then Apical Long-axis views
-
Apical 4-Chamber shows marked hypokinesis of the apical region (distal lateral wall and distal septum - LAD) with preserved contractility proximal lateral wall (LCx) and proximal septum (RCA). Estimated Ejection Fraction around 30%.
Apical 2-chamber shows apical hypokinesis, particularly along the anterior free wall (right side of picture - LAD) with preserved contractility towards the base (L main/prox LAD) and preserved contractility along the proximal inferior wall (left of screen - RCA).
Long-Axis images show poor contractility of the septum (right of screen - LAD) with preserved contractility to the proximal half of the posterior wall (left of screen - RCA/LCx).
In summary, marked regional wall motion abnormality affecting the entire apex, anterior septum, and anterior free wall suggestive of large LAD occlusion.
Preserved function of the proximal lateral wall on A4C, and proximal anterior wall on A2C suggest that the occlusion is distal to the left main (i.e. proximal LAD).
Thrombolysis was not indicated (pain over 12 hours) and Cath lab was available so the patient proceeded to urgent Primary PCI:
Angiogram
Proximal LAD occlusion (first video, top centre) which was opened with a drug-eluting stent with restoration of flow (second video).
Blood flow remained sluggish through the LAD due to large volume of damaged myocardium due to prolonged ischaemia.
POCUS Pearls:
Matching ECG territories to regional wall motion abnormalities can help confirm diagnosis of acute MI, particularly if a concerning ECG does not meet STEMI criteria.
Basic POCUS:
Aim to get a good parasternal view; in long (PLAX) and short (PSAX) axis. Start left of infraclavicular area and slide towards the left sternal edge 3rd-4th intercostal space. Marker pointed to patient’s right shoulder for PLAX (10-11 o’clock), and then rotate 90deg clockwise to get the PSAX (marker 2-3 o’clock)
A better view of the apex may be obtained by moving slightly lateral and dropping to the next rib space down.
Intermediate POCUS:
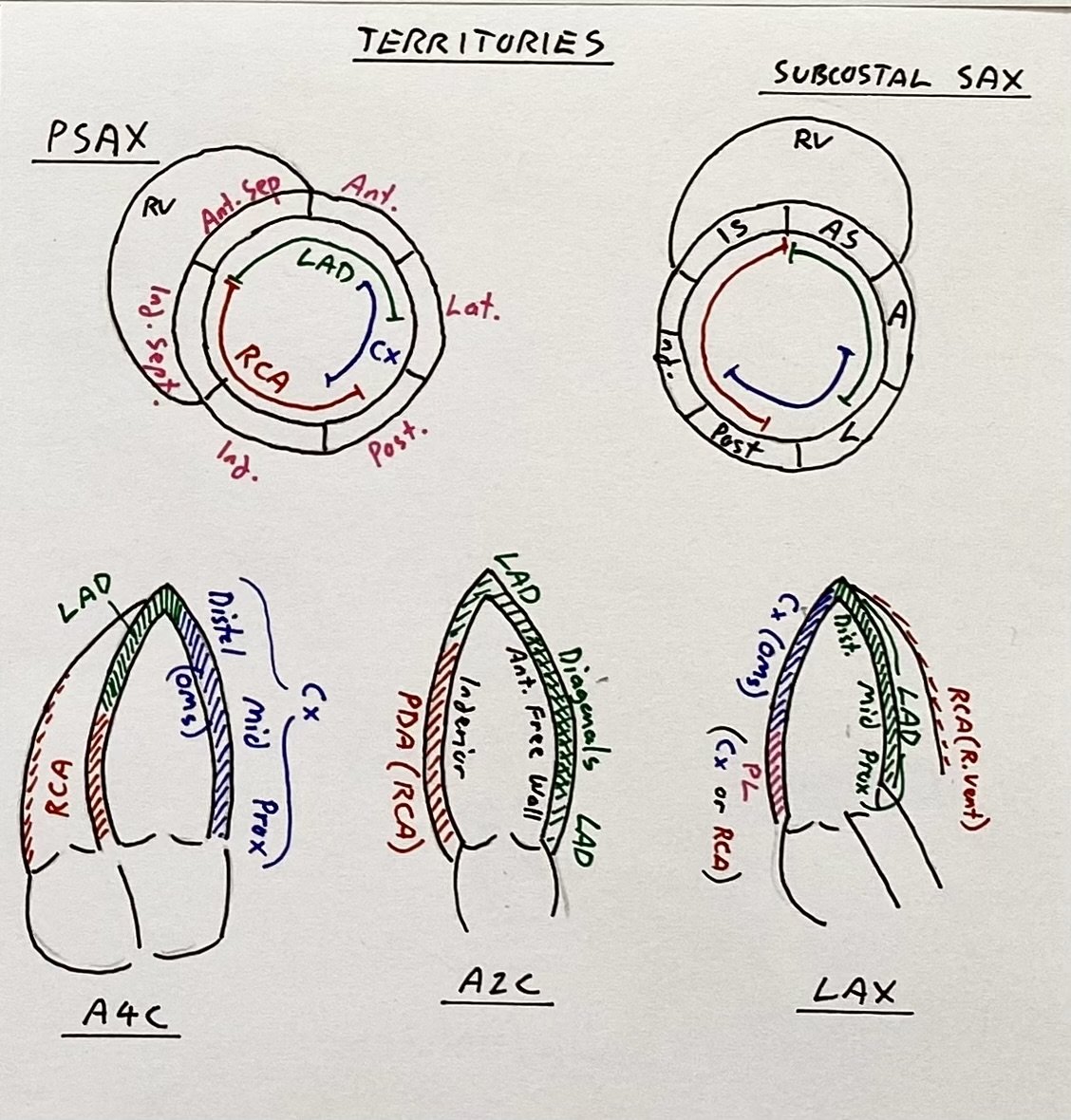
Three key views (Apical 4- and 2-chamber, and long axis) will visualise the key vascular territories (see right)
These should be confirmed with parasternal short-axis views.
In this case the large LAD and relatively small RCA/LCx meant that the whole apex was supplied by the LAD.
Vascular territories on the key Apical, and Short-axis views.
Extra Tips:
In delayed presentation of STEMI look for complications that may occur.
The echo also assessed for LV apical thrombus as well as for septal perforation
First video is a parasternal short-axis view assessing the apex for any thrombus
Second video uses colour across the inter-ventricular septum to ensure no septal perforation (would be seen as colour crossing the septum).
Case Conclusion
Patient developed acute pulmonary oedema from LV failure following reperfusion, was admitted to ICU where they required intubation due to ongoing respiratory failure.
Extra Tips:
Given the extensive anterior infarct, reduced EF (around 30%) and LV dysfunction affecting many segments, acute pulmonary oedema (APO) is not unexpected, so anticipate the need for respiratory support early by ensuring BiPAP is readily available.