Cardiology Case #2
Primary Author: Dr Alastair Robertson; Co-Authors: Dr Hywel James and David Law
Background
Male in his 40s presents with a 4 day history of progressive breathlessness & fevers. He has a background of known aortic regurgitation, heavy alcohol and cocaine use.
On assessment he is in respiratory distress (speaking phrases) and hypotensive.
RR 30, Sats 88% on air, HR 130, BP 94/76, temp 37.7, bilateral creps on auscultation
Initial ECG
Initial CXR
What is your first impression?
-
ECG:
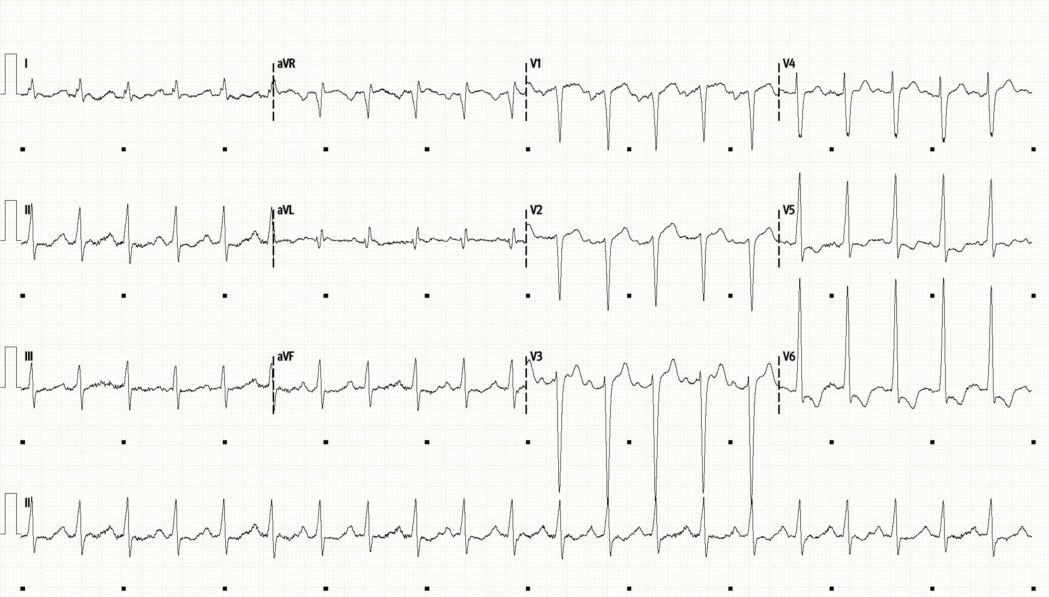
Sinus tachycardia with a rate of 130bpm. QRS width at upper limit of normal (100ms). LVH as signified by large-voltage QRS in precordial leads
Marked ST depression and T-wave inversion in V5 and V6, ST elevation in aVR suggesting some subendocardial ischaemia
An abnormal ECG, LVH and lateral changes raise the possibility of structural disease/cardiomyopathy whilst ST changes are also concerning for ischaemia (possible T1 MI or due to supply/demand mismatch)
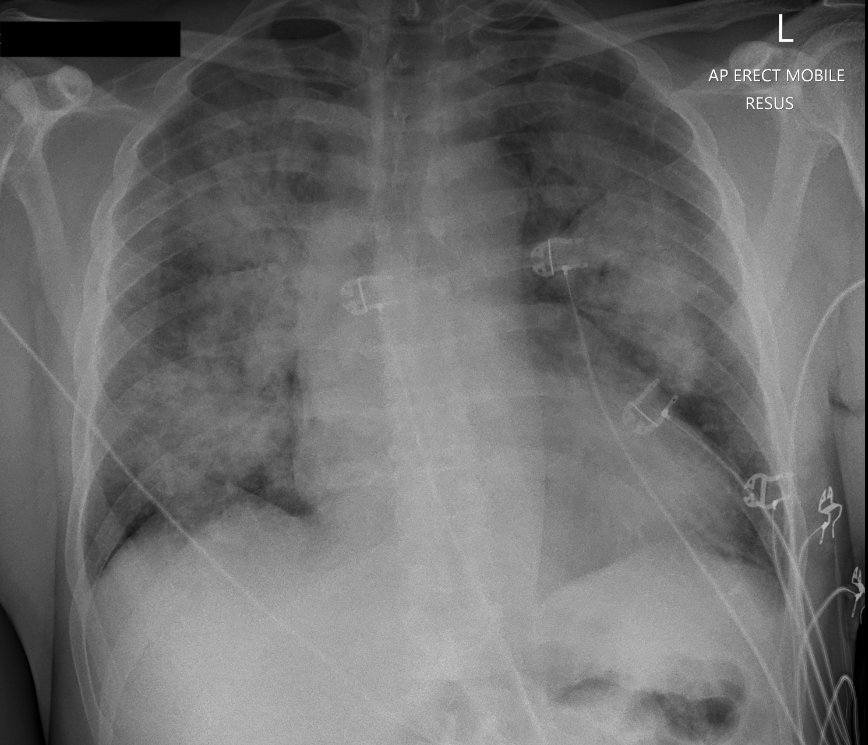
Chest XR:
Bilateral perihilar infiltrates/consolidation which could be due to pulmonary oedema (“batwing” sign) or infective process. Cardiomegaly allowing for AP film.
How much fluid do you give for his hypotension?
What is going on, what is the differential?
How could POCUS be useful?
You decide to pick up the ultrasound…
-
The PLAX view immediately shows a dilated cardiomyopathy. This is confirmed with the PSAX view of the LV base.
The LV is distended with hypertrophied, thickened walls. Contraction during systole is significantly impaired with an EF of approximately 10-15%.
PLAX shows the mitral valve is opening well but the aortic valve is calcified with restrictive movement (raises concern for stenosis and/or regurgitation.
There is no pericardial effusion (excluding pericardial tamponade as a cause of shock) and the RV size appears normal on the initial PLAX view.
POCUS Pearls
Use of POCUS immediately showed a severe dilated cardiomyopathy suggesting that respiratory distress is primarily from cardiac rather than respiratory pathology (or is at least a mixed picture).
This patient will not tolerate large volume IV fluid resuscitation given his decompensated cardiac failure.
Resuscitation should include respiratory support, cautious diuresis if haemodynamics will allow, and early use of inotropes/vasopressors over IV fluids to correct shock.
Basic POCUS
Again, the parasternal long axis is key. Start at the left sternal edge, 3rd/4th ICS with marker towards the patients right shoulder. You can quickly exclude pericardial effusion as well as assessing LV size/function as well as the RV size.
If you can get an apical view (see below) this also shows LV dilation and wall thickening. On this view you can see “smoke-like” wisps in the LV. This is SEC (Spontaneous Echo Contrast) which indicates blood stasis due to the poor LV function. It signifies an increased risk of LV thrombus.
Intermediate POCUS
Look at the videos below. Putting colour on the aortic valve shows a broad regurgitant jet - moderate/severe aortic regurgitation. This is seen in both the PLAX (top video) and the Apical 5-chamber (bottom video) views. Aortic stenosis is best assessed by the use of CW doppler through the valve in the A5C view.
In shocked states the degree of AS may appear artificially lowered due to poor cardiac output “low-flow AS” and must be reassessed once the patient is more haemodynamically stable.
Case Conclusion:
Bloods showed a static troponin of 170, a BNP of 15,000, and a CRP of 240.
He was stabilised on high-flow nasal prongs and admitted to ICU for BiPAP, vasopressors, and broad spectrum antibiotics. Viral PCR was subsequently positive for parainfluenza.
Formal TTE showed a bicuspid aortic valve with moderate/severe AS and AR and a dilated cardiomyopathy. Aetiology was thought to be cocaine-induced (+/- septic/alcoholic) cardiomyopathy compounded by congenital bicuspid AV pathology. His cardiac function slowly improved and was stepped down from ICU 10 days later.
Once stabilised he was diuresed and discharged on entresto, dapagliflozin, fuosemide, spironolactone and nebivolol.
Extra Tips:
Use of POCUS can rapidly help guide resuscitation in cases of undifferentiated shock and/or respiratory distress. It is also a rapid way to exclude pericardial tamponade.
BEWARE using isolated IVC assessment/measurement to guide fluid tolerance, particularly in patients who are sitting upright and/or on any form of PEEP - we will delve into this more in later cases
In this case, identification of a severe dilated cardiomyopathy and decompensated HFrEF avoided excessive IV fluid administration which would have worsened his cardiorespiratory function.
It is worth noting that increased LV wall thickness can be hard to appreciate on 2D echo when the ventricle is dilated such as it is here, so although wall thickness may appear normal there may still be LVH.