Cardiology Case #3
Authors: Dr Alastair Robertson, Co-Authors: Dr Hywel James and David Law
Background:
Gentleman in his 70s presents to ED with an acute onset of central chest pain with associated palpitations.
He has a background of paroxysmal AF and IHD. His medications include aspirin, clopidogrel and metoprolol but no other anticoagulation. Last echo on eMR was 10 years ago and was normal.
On assessment his pain has improved after IV fentanyl with NSWAS. He is stable. HR 140, BP 121/87, RR 19, Sats 98%, afebrile.
Initial ECG
Previous ECG from eMR obtained 2 years prior.
What is your interpretation of his ECG?
-
Regular tachycardia with a rate of around 140. Flutter waves are seen, particularly in V1. Thus the rhythm is most likely Atrial Flutter with 2:1 block (with 3:1 conduction noted at two points on the rhythm strip).
Right axis deviation with incomplete LBBB (QRS width around 100ms) and LPFB. Meets LVH voltage criteria.
Concave ST elevation in anterior leads V2 (1mm), V3 (2mm), V4 (1.5mm) is concerning for ischaemia but does not strictly meet STEMI criteria. Subtle ST depression/TW inversion in V6.
Of note Q waves are present in anterioseptal leads V1-4.
The old ECG shows sinus rhythm, borderline prolonged PR, normal QRS, and importantly no Q waves in anteroseptal leads.
Progress:
Serial hsTroponins are negative at 17 —> 18
He is given PO metoprolol, IV magnesium, and IV fluids with the aim of controlling his atrial flutter. Chest pain has largely resolved. How about cardioversion?
Due to concern for PE he goes for CTPA of which a slice is shown below.
What do you notice on the scan?
-
The study is negative for PE but a cirucular mass can be seen in the LV apex. This was called through with the differential potentially being tumour, or LV thrombus.
Cardiac POCUS
Parasternal Long-axis (top), Parasternal Short-axis of apex (middle) and Apical 2-chamber view of apex.
-
The Parasternal Long Axis view (first video) is busy. Directed by the CT result, the question is can we see an apical mass? It is present as an echogenic circular density in the LV cavity at the top left of the screen.
Also, when qualitatively assessing chamber sizes, the left atrium looks dilated which may be the cause of the atrial flutter. Both mitral and aortic valves are opening well, aortic root does not look dilated. RV size looks normal.
There is a significant left PLEURAL effusion as well as a trivial pericardial effusion. Pleural effusions will track deep (behind) the descending thoracic aorta on this view.
Contractility of the mid-anterior septum (LAD territory) is decreased with poor apical contractility. Overall LV function is moderately impaired.
The next two videos are a PSAX of the apex, and an apical view of the apex showing the large circular mass sitting in the LV apex. This was thought to be LV thrombus.
Both the PSAX and apical views show a bright white line in the LV wall at the apex which likely represents myocardial scarring from prior infarction.
POCUS Pearls
POCUS can be used to identify all of the relevant pathology in this case.
Basic POCUS
Start with a good Parasternal Long Axis -it is able to demonstrate multiple pathologies.
Initial depth of image is key. Optimise to 2-3 cm beyond the descending thoracic aorta. This will help identify a pericardial effusion and differentiate it from a pleural effusion.
Subsequently, decrease depth and assess LV and RV size as a ratio to each other. [LV 2/3, RV 1/3]
Assess overall LV function: grossly normal vs abnormal (hyperdynamic or reduced) .
The apical 4-chamber view (bottom video) shows both left and right atria are dilated consistent with significant mitral disease and likely cause of the atrial flutter.
For progression;
- Putting colour over the mitral valve (top video) shows a broad regurgitant jet. Moderate/severe MR will cause left atrial dilation which will predispose to atrial arrhythmias.
- Left atrial size can be measured in A4C (bottom video)
Intermediate POCUS
What has caused this LV thrombus ?
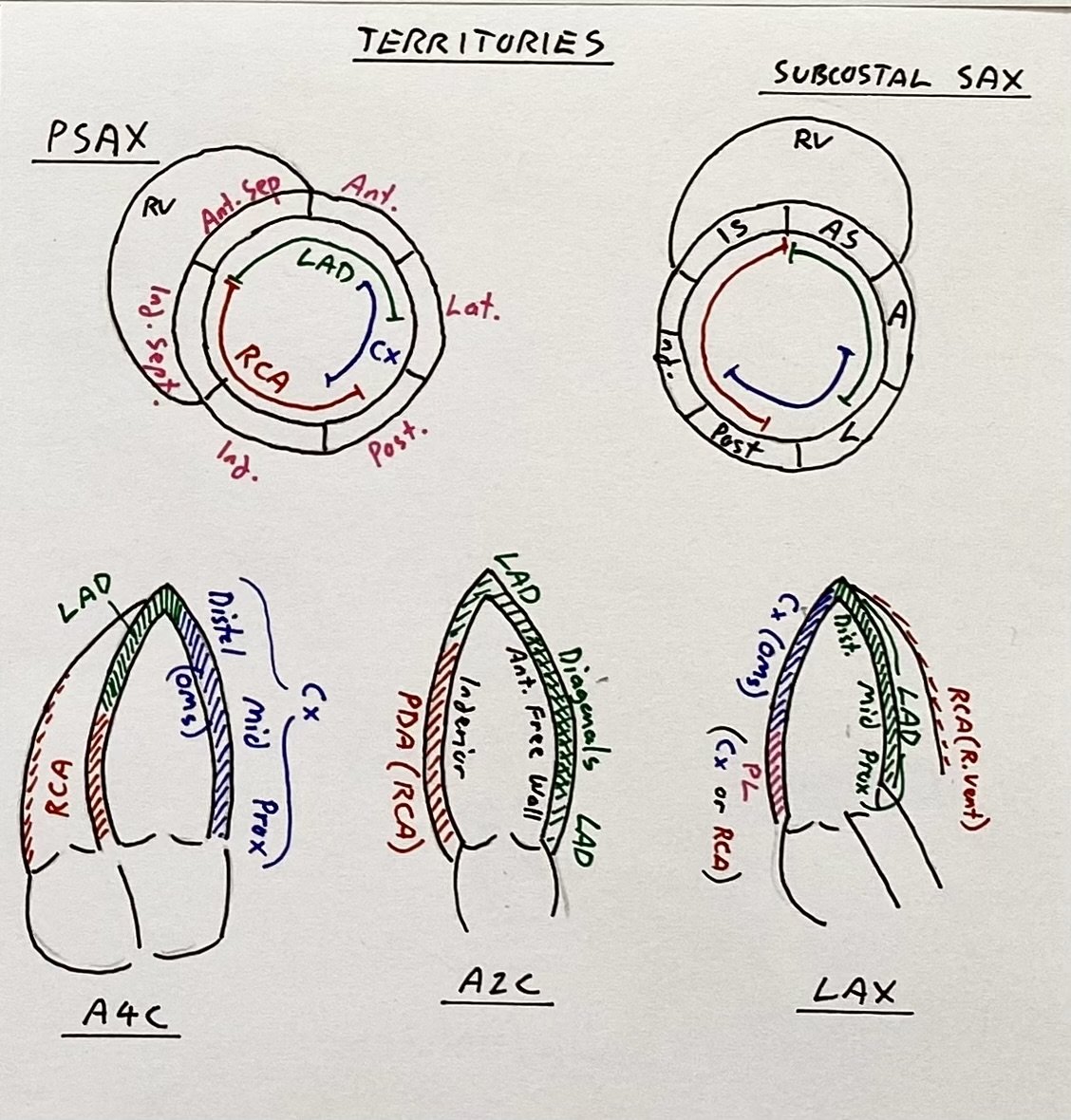
Images of the key vascular territories is important. Getting apical slices (A4-chamber, A2-chamber, and A long-axis) will cover the LV vascular territories. Then confirm with SAX views.
In the first video A4C the apex (generally served by LAD) is not contracting well. The lateral wall (right side, LCx territory) is contracting. The proximal part of the septum (left side, RCA territory) is thickening, but the distal septum (LAD) is not, with hyperechoic scarring.
The second video is an A2C. The left (posterior wall, RCA/PDA territory) is contracting well. On the right (anterior free wall) is also contracting reasonably well, except for the apex. This is supplied by the diagonals via the LAD.
The third video is an Apical Long Axis. The inferior wall (left side, RCA territory with some LCx distally) is working well until just before the very apex (LAD territory). The distal septum (right side, LAD territory) is contracting poorly, but the very proximal septum (bottom right, Left Main territory) is still contracting.
Recap the key Left Ventricle vascular territories (below) - apical hypokinesis fits with the LAD territory.
Given the anterior free wall (on A2C) is working, LAD occlusion likely occurred distal to the main diagonal branch. Thus, mid/distal LAD occlusion has caused the ischaemia, regional wall motion abnormality and apical scarring demonstrated.
This is reinforced by the ECG showing new established Q waves in the anteroseptal leads (LAD territory). POCUS confirms LAD territory hypokinesis with myocardial scarring and an LV thrombus.
Scarring and thrombus formation are delayed sequelae, raising the suspicion of a missed (silent) anterior MI LAD territory occlusion at some point since the previous ECG. The apical akinesis has caused an LV thrombus.
Remember in Case 1 (anterior STEMI from LAD occlusion) - it is worth assessing for LV thrombus with focussed apical views in the setting of anterior MI.
Left ventricle vascular territories on the key Apical, and Short-axis views.
Case Conclusion
The patient was initiated on a NOAC for treatment of his LV thrombus.
He remained tachycardic to around 140 overnight in ED. He was started on an amiodarone infusion, omiting the loading dose to target rate control rather than rhythm control. This was then switched to digoxin the following day.
He remained in flutter on CCU with a rate of over 100bpm for several days. His rate was eventually controlled on digoxin but he remained in atrial flutter. He was discharged with cardiology FU to monitor resolution of his thrombus.
Take home Tips
The key to differentiating pleural from pericardial effusions on the parasternal long axis is to identify the descending aorta (see below).
- - - Pleural effusions will sit behind (deep to) the aorta - - -
- - - Pericardial effusions will track in front of (anterior to) the aorta - - -
However both may be present.
Explore: look for pericardial effusions in other views; subcostal (probably the easiest, and the view used in an eFAST) or apical.
Lung base assessment (extended RUQ and LUQ views with curvilinear probe) as per an eFAST exam are useful to confirm pleural effusions.
Image from NephroPOCUS.com